How To Move A Hospital Bed
Affiliate three. Safe Patient Handling, Positioning, and Transfers
3.5 Positioning Patients in Bed
Positioning a patient in bed is of import for maintaining alignment and for preventing bed sores (pressure ulcers), pes driblet, and contractures (Perry et al., 2014). Proper positioning is also vital for providing condolement for patients who are bedridden or have decreased mobility related to a medical status or treatment. When positioning a patient in bed, supportive devices such as pillows, rolls, and blankets, forth with repositioning, can aid in providing condolement and safety (Perry et al., 2014).
Patient Positions in Bed
Positioning a patient in bed is a common procedure in the hospital. There are diverse positions possible for patients in bed, which may be determined by their condition, preference, or treatment related to an affliction. Table 3.6 lists patient positions in bed.
| Position | Description | ||
| Supine position | Patient lies flat on back. Additional supportive devices may be added for condolement. 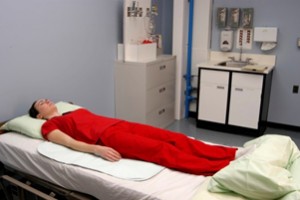 | ||
| Decumbent position | Patient lies on stomach with head turned to the side. 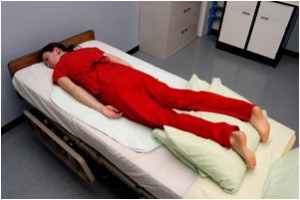 | ||
| Lateral position | Patient lies on the side of the trunk with the tiptop leg over the bottom leg. This position helps relieve force per unit area on the coccyx. 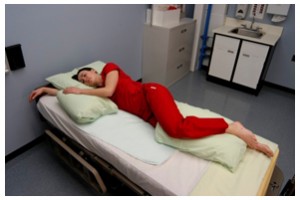 | ||
| Sims position | Patient lies between supine and prone with legs flexed in front end of the patient. Arms should be comfortably placed beside the patient, not underneath.  | ||
| Fowler's position | Patient's head of bed is placed at a 45-degree bending. Hips may or may not be flexed. This is a mutual position to provide patient condolement and intendance. 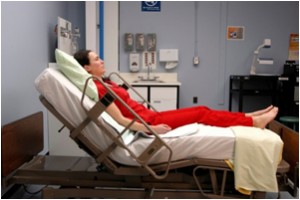 | ||
| Semi-Fowler's position | Patient's head of bed is placed at a 30-degree bending. This position is used for patients who take cardiac or respiratory conditions, and for patients with a nasogastric tube. 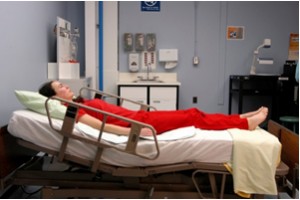 | ||
| Orthopneic or tripod position | Patient sits at the side of the bed with head resting on an over-bed table on top of several pillows. This position is used for patients with breathing difficulties. | ||
| Trendelenburg position | Identify the head of the bed lower than the feet. This position is used in situations such as hypotension and medical emergencies. It helps promote venous render to major organs such equally the head and heart. 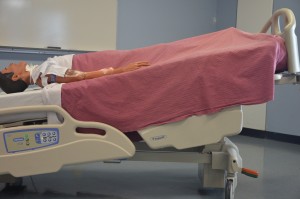 | ||
| Data source: ATI, 2015a; Perry et al., 2014; Potter et al., 2011 | |||
Moving a Patient up in Bed
When moving a patient in bed, perform a patient risk assessment prior to the procedure to determine the level of assistance needed for optimal patient care. If a patient is unable to assist with repositioning in bed, follow agency policy regarding "no patient lifts" and the use of mechanical lifts for complex and bariatric patients. Run across Checklist 25 for the steps to motility a patient up in bed.
Disclaimer: Always review and follow your hospital policy regarding this specific skill. | |||
Safety considerations:
| |||
Steps | Boosted Information | ||
| 1. Make sure an additional health care provider is available to assist with the move. | This procedure requires two health care providers. | ||
| 2. Explain to the patient what will happen and how the patient can help. | Doing this provides the patient with an opportunity to ask questions and help with the positioning. | ||
| 3. Complete risk assessment (Checklist 24) of patient's ability to aid with the positioning. | This step prevents injury to patient and health care provider. | ||
| 4. Raise bed to safe working pinnacle and ensure that brakes are applied. Health care providers stand on each side of the bed. | Principles of proper body mechanics assist prevent MSI. Condom working height is at waist level for the shortest health care provider. 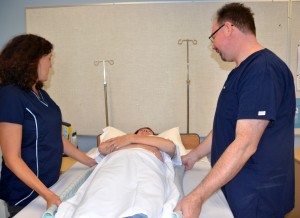 | ||
| 5. Lay patient supine; place pillow at the head of the bed and confronting the headboard. | This step protects the caput from accidentally hit the headboard during repositioning. | ||
| 6. Stand between shoulders and hips of patient, feet shoulder width apart. Weight will be shifted from back foot to front end foot. | This keeps the heaviest role of the patient closest to the centre of gravity of the health care providers.  | ||
| 7. Fan-fold the draw sheet toward the patient with palms facing up. | This provides a potent grip to motion the patient upwardly using the describe sheet. 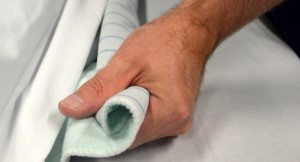 | ||
| 8. Inquire patient to tilt head toward chest, fold arms beyond breast, and bend knees to assistance with the movement. Allow the patient know when the move will happen. | This step prevents injury from patient and prepares patient for the movement. 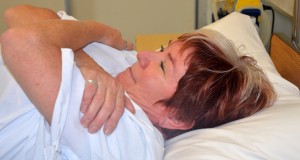 | ||
| 9. Tighten your gluteal and abdominal muscles, bend your knees, and keep dorsum directly and neutral. | The principles of proper body mechanics help prevent injury. | ||
| 10. On the count of three by the lead person, gently slide (not elevator) the patient up the bed, shifting your weight from the back foot to the front, keeping back straight with knees slightly bent. | The principles of proper trunk mechanics help preclude injury.  | ||
| xi. Supersede pillow under head, position patient in bed, and cover with sheets. | This stride promotes comfort and prevents damage to patient. | ||
| 12. Lower bed, raise side track as required, and ensure call bell is within attain. Perform paw hygiene. | Placing bed and side rails in safe positions reduces the likelihood of injury to patient. Proper placement of call bell facilitates patient's ability to ask for assistance.  Manus hygiene reduces the spread of microorganisms. | ||
| Data source: Perry et al., 2014; PHSA, 2010 | |||
Sentinel these iii videos for more information about how to motion a patient upwards in bed.
Take this Repositioning a Patient in Bed, Caregivers at Head course to learn how to move a patient up in bed, with caregivers at the head of the bed.
Have this Repositioning a Patient in Bed, Caregivers Facing Each Other course to learn how to move a patient up in bed, with the caregivers facing each other.
Have this Repositioning a Patient in Bed, Diagonal Technique course to larn how to motility a patient up in bed, with the caregivers standing positioned diagonally.
Positioning a Patient to the Side of the Bed
Prior to ambulating, repositioning, or transferring a patient from one surface to another (e.g., a stretcher to a bed), it may be necessary to move the patient to the side of the bed to avoid straining or excessive reaching by the health care provider. Positioning the patient to the side of the bed also allows the health intendance provider to have the patient as close as possible to the health care provider's center of gravity for optimal residuum during patient handling. Checklist 26 describes how to safely movement a patient to the side of the bed.
Disclaimer: Always review and follow your hospital policy regarding this specific skill. | |||
Prophylactic considerations:
| |||
Steps | Additional Information | ||
| one. Make sure you have as many additional health care providers as needed to aid with the movement. | The procedure works best with two or more wellness care providers, depending on the size of the patient and the size of the wellness care professional. | ||
| 2. Explain to the patient what volition happen and how the patient can help. | This provides the patient with an opportunity to inquire questions and help with the positioning. | ||
| three. Raise bed to prophylactic working height and ensure that brakes are applied. Lay patient supine. | Principles of proper torso mechanics help prevent MSI. Safe working acme is at waist level for the shortest health intendance provider. | ||
| 4. Stand on the side of the bed the patient is moving toward. One person stands at the shoulder area and the other person stands near the hip area, with anxiety shoulder width apart. | This step keeps the heaviest part of the patient closest to the center of gravity of the wellness care providers. 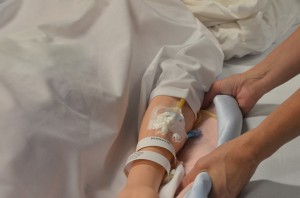 | ||
| five. Fan-fold the depict canvas toward the patient with palms facing upwards. |  | ||
| 6. Have the health intendance provider at the head of the bed grasp the pillow with one hand and the depict sheet with the other manus. | This prevents injury to patient. 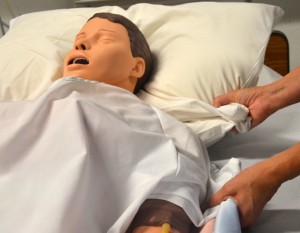 | ||
| seven. Accept patient place arms across breast. | This pace prevents injury to patient.  | ||
| viii. Tighten your gluteal and abdominal muscles, curve your knees, and keep back straight and neutral. Identify one foot in forepart of the other. The weight volition shift from the front end pes to the dorsum during the motion. | Utilize of proper body mechanics helps prevent injury when handling patients. | ||
| 9. On the count of iii by the lead person, with arms tight and shoulders down, shift your weight from the front pes to the back pes. Use your large leg muscles to movement the patient. Do not elevator, only gently slide the patient. |   If the patient is bariatric, the move should be repeated to correctly position the patient, or use a mechanical lift. | ||
| 10. Once patient is positioned toward the side of the bed, ensure pillow is comfortable nether the head, and straighten sheets. Complete all other procedures related to prophylactic patient handling. | This step promotes comfort and prevents harm to patient.  | ||
| 11. Lower bed, raise side rails as required, and ensure telephone call bell is within achieve. Perform paw hygiene. | Placing bed and side rails in safe positions reduces the likelihood of injury to patient. Proper placement of call bell facilitates patient's power to ask for assistance.  Paw hygiene reduces the spread of microorganisms. | ||
| Data source: Perry et al., 2014; PHSA, 2010 | |||
- Name five body mechanic principles that should be used when moving a patient upwards in bed.
- A wellness care provider completes a hazard assessment for a patient and determines the patient is unable to assist with repositioning. What should the health care provider do next?
- Your patient is experiencing shortness of breath related to center failure. Which position in bed is best for this condition?
Source: https://opentextbc.ca/clinicalskills/chapter/3-4-positioning-a-patient-in-bed/

0 Response to "How To Move A Hospital Bed"
Post a Comment